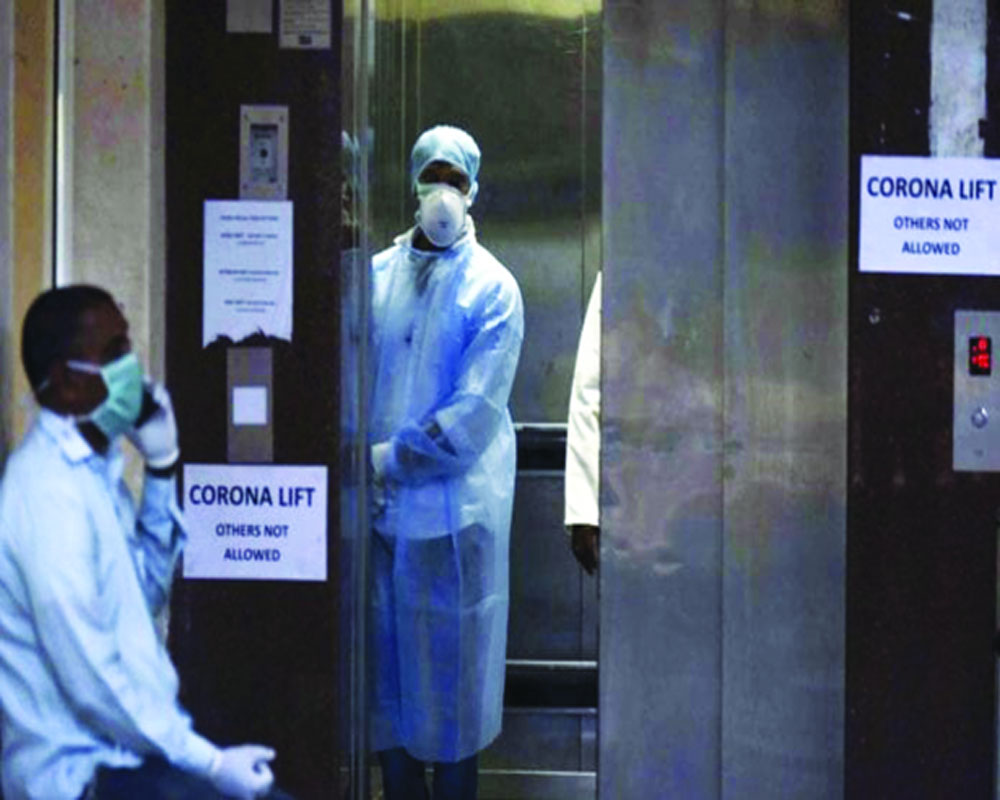
Our own safety net
by Opinion Express / 03 April 2020As we run against time in our battle to fight the virus, we need to scale up domestic manufacture of medical devices
The Coronavirus spiral was inevitable but now that it is squeezing health infrastructure and medical care staff, we are battling a second front of the disease, when it attacks the preparedness. Doctors and care-givers from around the country have complained, even threatened to go on strike, because they do not have enough personal protective equipment (PPE), namely coveralls, gloves, goggles, masks and so on. There have been reports of frontline staff making use of raincoats and anything else that they can lay their hands on. The lockdown and the migration of labour have meant that even those manufacturing these essential gear are not being able to roll them out at breakneck speed. Though there is no dearth of Indian innovation — like the Pune virologist’s version of the test kits, IITs’ collective efforts to roll out apparatus or even car companies’ offer to make ventilators — the fact of the matter is these are all small-scale efforts. What is needed is a massive rollout, which, because of policy hurdles, delay in placing orders and over-dependence, like the West, on China for crucial components, has been halted badly. Even the contracts being handled by domestic companies are of a small to middling nature, with no capabilities to scale up output. It would be easy enough to attribute the scarcity to a global trend, arguing all countries battling the coronavirus are facing it as well. But we didn’t plan it as well with the Government ordering PPEs just before the lockdown. Safety wear would now need at least three weeks to be readied domestically, considering imports are not that reliable with most infected countries dependent on factory floors in China and Southeast Asia. China has just about emerged after the first wave of the virus and its manufacturing prowess is still not 100 per cent. The Government could also not have exported 90 tonnes of medical equipment and safety gear to Serbia at this time of a national emergency, confirmed by a tweet from the United Nations Development Programme (UNDP) though denied by the Health Ministry. Leave aside N95, even the triple layer surgical masks are not available for healthcare staff. There is also the issue of facilitating working capital for these units in the time of lockdown. As for chemicals and disinfectants, India has been dependent on China for critical intermediate goods and components. With so much dependence on China, particularly for raw materials, it is difficult to find easy replacements.
As we ride this unprecedented World War III, that literally came from nowhere and hit us before we could realise it, what should be the road looking ahead? Simply prioritise our health sector and go back to home-grown drug and health equipment manufacturing. They were there before but globalisation meant these units were sidelined and lost out on the cost advantage to cheaper imports. And now that the virus may spur the process of de-globalisation as it were, we need to begin with crucial sectors that impact national safety, health and well-being. Immediately after Wuhan, the Government drew up a list of 38 drug raw materials that it wants locally produced to end the country’s dependence on Chinese imports. Some of our key life-saving drugs, including those for cardio-vascular issues, use active pharmaceutical ingredients (APIs), which are solely sourced from China. Indian drugmakers import around 70 per cent of their total bulk drugs from China. Now there is no time for committees, policy or pondering. There is already a Make in India wishlist suggesting ways to make India one of the top five medical devices manufacturing hubs in the world. Most domestic manufacturers have in pre-crisis days shut their idling units and become importers and traders themselves. We have ignored an industry that could have helped us stave off this crisis. What else explains that though there are 1,000 domestic medical devices manufacturers, only 15 have a turnover of above Rs 200 crore and the rest are less than Rs 10 crore. If they are to scale up, then they need an enabling ecosystem, a level-playing field vis-a-vis imports and assured volumes. The last won’t be difficult given India’s huge market for healthcare, projected to be the fourth largest in Asia. Post-Corona, the demand is not expected to dip but rise. This way we can easily end our import dependence by 70-90 per cent. And be self-sufficient in the time of unforeseen crisis.
(Courtesy: The Pioneer)

Covid 19 – Going for broke
by Deepak Sinha / 23 March 2020In a country with our population density to claim that hundred per cent source identification or tracking is even feasible is akin to believing in Santa Claus
We are going through a time of uncertainty, fear and gloom, though stories of human resolve, courage and sheer determination do give us hope for the future. We live in unprecedented times of which we have no previous experience, little knowledge and even lesser understanding. There are none here who have survived either the Spanish flu pandemic of 1918 that killed 33 million people (including approximately six million from the sub-continent) or the Bengal famine of 1942 that killed 10 million. What is, however, absolutely clear is that we are in a global war against an unforgiving and unseen enemy who respects no borders, ethnicity, class, age, religion or caste.
If we are to beat this enemy, not just physically but psychologically, socially and economically as well, we have no choice but to work together as a global community and act with compassion, forbearance and courage not just in our own self-interest but for the community at large. It finally boils down to this, if we are to call ourselves civilised. Most importantly, the time for political posturing or playing games is way past. In war, as is often said, there is no place for the runners-up.
If the information available in the public domain is to be believed, the Government has done a sterling job in limiting infections and fatalities for now, through its rapid response. Unfortunately, the figures being bandied about are coming in for increasing scrutiny for a variety of reasons. The question of what is the policy governing testing and how many tests are being done is at the crux of the controversy.
As per information available in the public domain, the existing capacity to test for the virus is 500 per day, which is being ramped up in the coming days. Thus, at present only those coming from affected countries are being screened and if their condition seems doubtful, are being tested. Those cleared in screening are expected to undergo either supervised or self- quarantine before being allowed to mingle. Tests are also being done on those who may have fallen sick after coming in contact with someone returning from abroad. In addition, the Government has also done 800 tests as on date on random patients across the country who, are at present admitted in hospitals with acute respiratory disorders.
On the basis of these tests having turned up negative the Government insists that there have been no cases of community spread. Therein lies the rub, as many known positive cases, leave aside those who are asymptomatic, have deliberately escaped from quarantine, no doubt infecting those they may have subsequently come in contact with, who in turn will infect others, which is what community spread is all about. In a country with our population density to claim that hundred per cent source identification or tracking is even feasible is akin to believing in Santa Claus. Of course, there is the possibility that the Government is aware of the true picture and hiding it from the public to avoid any onset of panic.
If that be the motivation, the Government is making a huge error as most of us are well aware as to what is happening in different parts of the world. As a matter of fact, conservative studies on the subject suggest that actual cases are about ten times the numbers that have been identified and given that the cases are doubling every three days, the number of people infected will be 1,024 times the present number within a month as simple mathematics suggests. This in our context, with total identified cases as 169 as on March 19 that has increased by one-third along expected lines on the March 20 will, in all likelihood, range between 1.7 lakh and 17 lakh by April 19, depending on which figures we wish to believe, if we do not take further steps that are needed to halt the spread. From within these numbers, as seen elsewhere, 15 per cent will require Intensive Care Unit facilities and two-three per cent will not survive.
The problem with hierarchies and the bureaucracies that run them is that they abhor vacuums, as that condition requires them to assert themselves, avoid accountability for obvious reasons and can only think and act linearly given their long-standing ethos and organisational architecture. An emergency of this kind requires lateral thinking, taking of risks and forceful interventions, all of which fall in the realm of the political leadership that now needs to step forward, provide clear directions, impart the momentum required and most importantly, accept accountability. While Prime Minister Narendra Modi has certainly shown his interest in assuming a leadership role his known dependence on the bureaucracy is a distinct disadvantage at this time.
Thus we have adopted the bureaucratic playbook to tackle the issue. As a result our response has been bureaucratic, admittedly much quicker but still along plodding linear lines with each agency and department attempting to show how efficiently they are handling challenges that they face. Forget the “All of country” model that is absolutely necessary, we have not even been able to put an “All of Government” approach in place. This is best brought out by the Prime Minister’s address to the nation on March 19. It was a motivational talk with no substantive future course of action being announced, except for a voluntary one day national “Janta (public) curfew”, which probably will be a harbinger of tougher measures in the future. In all truth, the time for motivational talks is long past, what we now need is a general who will lead us into battle. Moreover, such an approach is unviable, because by the time we take the next step another week would have passed and numbers of those infected quadrupled, adding to avoidable stress on our healthcare system and to fatalities.
It is essential that our political leaders and the average citizen comprehend the nature of the beast that we are at war with and face facts that have either emerged from experiences elsewhere or are peculiar to our situation. First, there is no getting away from the fact that we have a population of 1.3 billion and the cost of testing and providing the necessary support facilities are humungous. Obviously, no Government, whatever its efficiency, can ever provide cover for all our citizens. Second, social distancing, which include forcible quarantine, despite its flaws, appears to have emerged as the only viable alternative for keeping the Coronavirus under check and in reducing the rate of infection, till a suitable remedy is found.
The world around us has completely changed and yet we seem to be living in a time warp, hoping to avoid having to face the dragon that has felled much of the world. Let us face reality and accept that in these circumstances there is no time for half measures. Imposition of Section 144 of the CrPC, as has been done in some places, or hoping to enhance testing facilities in the coming days, which in any case is unavoidable, are measures that are simply not enough and are just too little and too late. In military terms, we need to launch an immediate blitzkrieg and in fact, have little choice but to immediately adopt measures that the Chinese and Italians did only as a last resort.
It is essential that a nationwide curfew for a minimum of 14 days be declared soonest along with other measures such as reducing the frequency of mass transit systems, banning taxis and only permitting minimum essential personnel to move out of their homes.These measures must be strictly implemented by deploying the military, assisted by the Central Armed Police Forces (CAPF), on the streets. While these are harsh and desperate measures with dire economic implications, we have no option, as we will otherwise find ourselves overwhelmed with the possibility of serious social disruptions.
Undoubtedly, the biggest problem will be faced by those whose very livelihood is dependent on their daily earnings. As in any major natural disaster this would require the Government to provide the requisite relief to all those impacted at their place of residence. This in effect requires that the armed forces be fully mobilised and deployed and tasked for conducting internal security and humanitarian and relief operations.
Time is of the essence here and discussions and committees have little meaning now and in fact these measures needed to have been implemented yesterday.
To enable the military to mobilise and deploy would require a minimum of three-four days, in which time we must remember, the numbers of those infected would have doubled. Implementation of such measures with a warning period will also allow citizens to stock up on essentials. For those who believe that such drastic action is uncalled for, would do well to study the impact of a graduated response in countries like Italy, Spain, the United States and France. By going for broke, if nothing else, we would certainly avoid much of the stress that the healthcare infrastructure of those countries were put through, infrastructure that we are woefully short of and have little ability to scale up.
(Writer: Deepak Sinha; Courtesy: The Pioneer)

Indo-China row on Corona virus
by Opinion Express / 25 February 2020Beijing’s selective engagement with India on the Wuhan evacuations is plain confrontationist
Desperate times call for desperate measures and when a global crisis has a new name called Coronavirus with a hydra-headed manifestation, then politics should be the last concern between nations who must unitedly fight it. Unfortunately, China, which is filtering the extent of its health crisis lest it be construed as bad propaganda for its global stakes, has let that unease creep into its bilateral ties with India. Seems like the spiralling epidemic has torn the “relative calm” in the strategic partnership. A spat that could have been settled by discussion and mutual understanding has unnecessarily been allowed to gain traction. The current row stems from China’s refusal to grant permission to our military aircraft for the evacuation of several Indians from the Coronavirus-hit Wuhan. Although China facilitated the civil flights by rescue missions, it is dragging its feet over clearances for this one, attributing it to procedural norms given the disease has reached a higher degree of criticality. But India maintains that it is precisely because of this and its responsibility to protect its citizens that it was sending in the C-17 Globemaster, equipped with medical facilities, to bring back Indians, assuming they were infected. Yet in a tit-for-tat response, Beijing accused New Delhi of being selfish and holding back essential medical equipment required by local authorities and medical workers for treating patients. More, China has called upon the Indian authorities to follow the World Health Organisation (WHO) guidelines that call for resumption of all trade and personal exchanges with it to restore normalcy. Yet the world knows that when it comes to humanitarian missions, India has never held itself back. So this strong-arm and negotiatory tactics by the Chinese are not warranted. In all this bickering, not least unexpected, the Chinese response was the same as it was during the outbreak of the virus, “denial.” So the fate of around 100-odd Indians, who remain stuck in the Chinese city, is still undecided.
Besides, Beijing cannot justify its “selective” engagement with India on the evacuation process, allowing permission to some while denying it to others. As it turns out, in the same “critical period,” three other nations were allowed to operate their evacuation flights. What is incomprehensible is that just a few days ago, the Chinese authorities applauded the “kindness” shown by New Delhi in helping them tackle the outbreak. Premier Xi Jinping had himself lauded India for offering solidarity and assistance. The mixed messages are typical of the larger Chinese strategy of keeping us on our toes by speaking in a forked tongue. Despite this blow-hot-blow-cold attitude of the Chinese, the Indian Government chose to keep differences aside and sought to aggressively push itself to help China contain the virus. From agreeing to test clinical samples from abroad in its laboratories to offering help with the evacuation of people from affected areas to lifting the ban on the export of personal protection equipment — it has done it all. The least one could have expected of the Chinese, given their continued emphasis on strategic relationship and intention to look at trade and other broader areas of cooperation, was to acknowledge the role played by other nations, including India, in fighting the epidemic. But that’s too much to ask from it. In all the three sorties carried out to date, where more than 600 Indians have been airlifted, working with China has been a nightmare with the biggest hurdle coming by way of getting approvals from its authorities — Central, provincial as well as local. It must also not be forgotten that ripple effects of the spread of the virus are being felt in India, as in other nations. We, too, need to be prepared to tackle any potential crisis. India’s stand with regard to restrictions on some medical devices assumes prominence on account of our fast depleting stocks and low domestic output. In fact, the crisis has led to the deep realisation of how we are heavily reliant on the Chinese for the procurement of raw materials and key ingredients for the production of medical equipment and drugs. So much so that the Government is all set to create new opportunities for Indian firms to emerge as an alternative producing destination to fill the supply vacuum. This outbreak should serve as a warning for Indian industries to diversify their supply chains and encourage the production of critical components within India. Till we are dependent on supplies from China, it will use our weakness to leverage diplomacy.
(Courtesy: The Pioneer)

Public Health Sector : New Area Of Study
by Opinion Express / 08 May 2019We have all heard the adgage — prevention is better than cure. Public health deals with prevention and control of diseases. It involves researching and educating people how to prevent or manage health issues. People interested in Science and want to serve the society, a career in public health is the way forward. The field of public health is varied and has many academic disciplines ranging from pure research to direct public education. To work in public health sector a master’s in Public Health is appropriate. One can also explore degree programmes in healthcare administration or community health. A few more colleges to study are:
Emergency Management and Research Institute, Secunderabad. Course: Advanced PGD in Emergency Care
Indian Institutes of Public Health, Gandhinagar, Ahmedabad. Course: Associate Fellow in Industrial Health
SRM Institute of Science and Technology: School of Public Health, Kancheepuram. Course: Associate Fellow in Industrial Health
Medvarsity Online Limited, Hyderabad. Course: Diploma in Family Medicare
Writer: Pioneer
Courtesy: The Pioneer
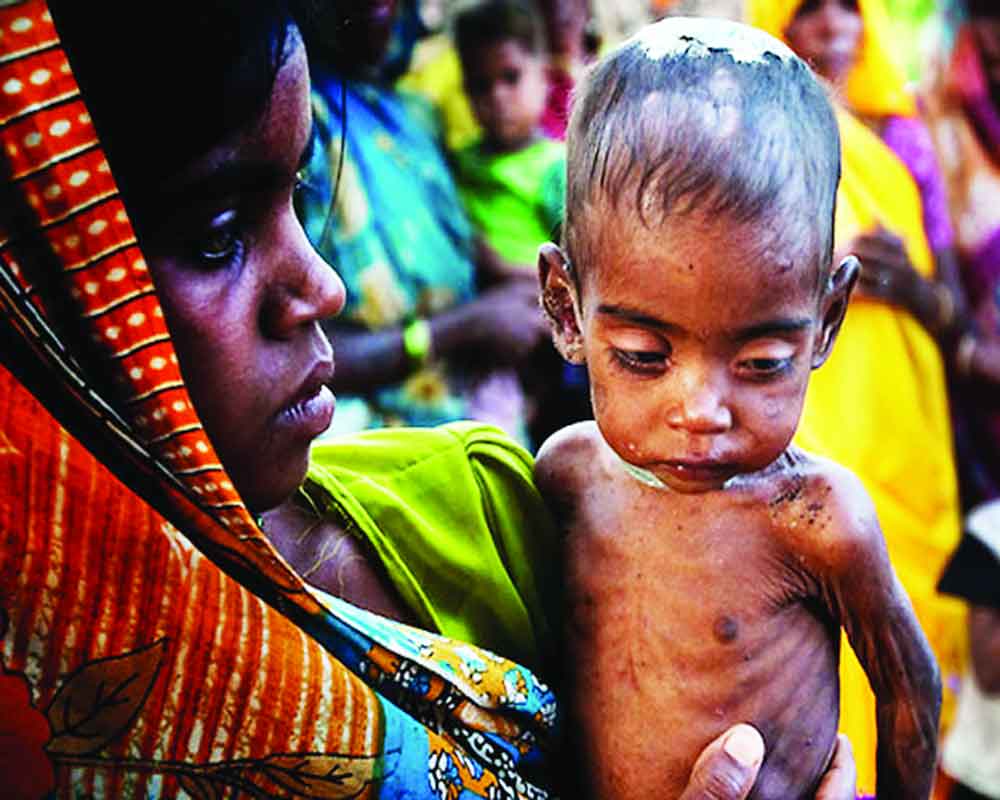
All About POSHAN: “Prime Minister’s Overarching Scheme for Holistic Nourishment” Abhiyaan
by JP Nadda / 05 February 2019Malnutrition has been a public health issue in our country for which Prime Minister Narendra Modi has set the agenda through the POSHAN (Prime Minister’s Overarching Scheme for Holistic Nourishment) Abhiyaan. He has announced clear targets and visible results to be seen by 2022, the 75th anniversary of the country’s Independence. The aim is to improve nutritional outcomes for children, pregnant women and lactating mothers. The targets under the POSHAN Abhiyaan are to reduce stunting, under-nutrition, anaemia (among young children, women and adolescent girls) and bring down low birth weight by two per cent, two per cent, three per cent and two per cent per annum respectively. Additional efforts will be made to bring down stunting from 38.4 per cent (NHFS-4) to 25 per cent by 2022. With this commitment from the highest level of leadership, nutrition is a clear priority for this Government.
India’s National Health Policy (2017) as well as the National Nutrition Strategy (2017) recognise that anaemia, which is a result of iron deficiency, has harmful consequences for maternal and child survival and overall productivity of the nation. Anaemia affects roughly one-third of the world’s population. Those with anaemia have low immunity and work productivity. It adversely impacts cognitive development of children. Anaemia in pregnant women is more likely to increase the risk of post-partum haemorrhage, low-birth weight babies, pre-mature birth, still birth and maternal death.
According to the National Family Health Survey-4 (2015-16), anaemia prevalence across all ages is extremely high in India. The percentage of children, aged between six and 59 months, having anaemia is a whopping 58 per cent while the percentage of women of reproductive age having anaemia is 53 per cent. As much as 50 per cent of pregnant women at any given point of time have anaemia.
There are many causes of anaemia but iron deficiency accounts for close to 50 per cent of cases among school children and women of reproductive age group and 80 per cent in children between two and five years of age (UNICEF and WHO Joint Statement 2001). Infectious diseases such as malaria, helminth infections, TB and hemoglobinopathies are other causes that contribute to the high prevalence of anaemia.
Unlike earlier attempts made to tackle the issue, there is a convergence of various departments and Ministries to achieve the desired results under the anaemia-mukt Bharat strategy. It is pertinent to note that the programme is being implemented pan- India, involving the community. Reaching out to everyone, particularly the vulnerable sections, is an integral strategy under POSHAN Abhiyaan. For this, the Government has improved and strengthened service delivery to ensure an efficient supply chain, encouraged use of technology to reach the targetted beneficiaries and bring about behavioural change through professional counselling.
Anaemia-mukt Bharat is a critical component of the POSHAN Abhiyaan and is expected to benefit 450 million people by 2022. It is based on six interventions, including prophylactic iron and folic supplementation; deworming and behaviour change campaign focussing on key behaviours such as appropriate infant and young child-feeding practices; increased intake of iron-rich diet or fortified food; ensuring delayed cord clamping after delivery; anaemia testing by using digital methods with special focus on pregnant women and adolescents and finally, screening and treatment of non-nutritional causes of anaemia in endemic pockets, malaria included. The strategy focusses on testing and treating anaemia in school-going adolescents and pregnant women using newer technologies, establishing institutional mechanisms for advanced research in the condition and a comprehensive communication strategy.
Considering that there are several other determinants of nutrition, linkages with other initiatives of the Government have been established. The Swachh Bharat Abhiyan focuses on creating open defecation-free communities that impact the rates of diarrhoea and gut infections among children. The Pradhan Mantri Matritva Vandana Yojana provides monetary support to pregnant women and lactating mothers for adequate diet, which in turn, promotes health-seeking behaviour.
Mission Indradhanush is increasing the rate of complete immunisation of women and children while the Mother Absolute Affection (MAA) programme is a nation-wide initiative to improve infant and young child-feeding practices. The Pradhan Mantri Surakshit Matritva Abhiyan (PMSMA) ensures quality ante-natal care for pregnant women, while the school children are being screened annually for diseases and nutritional deficiencies under the Rashtriya Bal Swasthya Karyakram (RBSK).
The Ministry of Health and Family Welfare is collaborating with the Ministry of Women and Child Development (MoWCD) on activities to be carried out during the POSHAN Maah that is observed in September every year. As part of the POSHAN Maah, 2018, AIIMS, New Delhi, along with six regional centres (Rajasthan, Madhya Pradesh, Odisha, Bihar, Chhattishgarh and Uttarakhand) undertook intensive BCC along with test and treat campaigns focussed on WRA (15-49 years) and under five children.
Also, our initiative, Village Health Sanitation and Nutrition Day (VHNDS), has been strengthened to be observed as ‘POSHAN Melas’ and are being leveraged as an opportunity to reach out to the community for counselling on health-seeking behaviours. Besides VHNDS, collaborating activities with MoWCD include traditional practices such as ‘Godbharai’ and ‘Annaprashan’ as part of POSHAN Abhiyaan for increased acceptance and involvement of the community.
Providing iron and folic acid supplementation and treatment to high risk groups, prevention and treatment of communicable diseases, promoting consumption of all micro-nutrients, and more importantly, encouraging birth spacing through the use of contraception are some other initiatives being taken by the Government for a holistic and life-cycle approach to the issue.
Implementing a programme of this magnitude is by no means an easy task but the Government is committed to end the scourge of anaemia and under-nutrition by rolling it out as a jan andolan (public movement). The decline in the prevalence of anaemia will contribute in improved maternal and child survival and improved health outcomes.
(The writer is Union Minister of Health and Family Welfare)
Writer: JP Nadda
Courtesy: The Pioneer

2019: The Year to Ensure Better Health Initiatives
by Opinion Express / 02 January 2019Last year was eventful for public health in India as the government followed up on some of its key decisions announced before. Ayushman Bharat was launched to implement select recommendations made in the National Health Policy (2017). The Mental Healthcare Act, 2017, was implemented while the Insurance Regulatory Development Authority (IRDA) mandated that mental health problems would henceforth be a part of insurance schemes. Several new health-related decisions were also taken — a series of approvals by the Union Cabinet, new bills for consideration by Parliament and setting up new medical colleges in various States. However, there is always a time lag between an idea translating into policy and programme. The initial discussion on health and wellness centres had started in 2013. The precursor of the Pradhan Mantri Jan Arogya Yojana (PMJAY) was the National Health Protection Mission, which was originally announced in 2016. Ayushman Bharat itself took off from the earlier discussion on National Health Assurance Mission of 2014 among others. The country has already suffered because of a laid-back attitude followed by a slow-paced implementation. Building upon what started in 2018, here is a wishlist for 2019.
Build on Ayushman Bharat programme: Ayushman Bharat, which was announced on February 1, 2018, was inarguably a major public health programme of the Union Government after the National Rural Health Mission (NRHM) in 2005. The Ayushman Bharat programme, with two components of health and wellness centres (for strengthening primary healthcare) and Pradhan Mantri Jan Arogya Yojana (for secondary and tertiary level hospitalisation) were credited for placing health higher on the political agenda. Yet, public health experts and journals alike continued to make the mistake of equating Ayushman Bharat with PMJAY, often forgetting that the health and wellness centre component is foundational for the success of PMJAY as well. It was not without reason that health and wellness centres as envisaged in Ayushman Bharat were launched on April 14 last year at Bijapur, Chhattisgarh, months before PMJAY was launched on September 23, 2018 at Ranchi, Jharkhand.
Much of 2018 was spent on planning for scaling up the healthcare scheme, so this year should be utilised for an accelerated implementation. More attention should be paid to getting more health and wellness centres going through state-specific innovations and increased utilisation of a range of service packages under PMJAY, especially in greenfield states, with efficient mechanisms for fraud detection. It will serve well if a detailed roadmap and execution plan for Ayushman Bharat is developed with proper funding, approved and placed in public domain, which will enhance its accountability at various levels.
States showing leadership in better health regimes: Towards the end of the year, the Uttarakhand government launched the breakthrough Atal Ayushman Uttarakhand Yojana, which covers 100 per cent of the State’s population compared to the proposed 40 per cent in Ayushman Bharat-PMJAY. Health is a State subject in our country and the success of any initiative by the Centre is largely dependent upon the additional inputs by the States. This year, we expect Karnataka, Meghalaya and Punjab to also take the lead and announce similar total population coverage under PMJAY. Besides this, it would be reasonable to expect that the newly-elected Government at the Centre in May extends the coverage with AB-PMJAY from the existing 40 per cent families to an additional 20 per cent of families. It should also announce a roadmap to cover 80 per cent or more population by 2022.
Basti dawakhanas in Hyderabad: The Greater Hyderabad Municipal Corporation (GHMC), in collaboration with the Telangana Government, launched 17 basti dawakhanas (or slum health clinics) in Hyderabad in April 2018. These facilities in the State are inspired by the mohalla clinics of Delhi and comprise the first urban local body-led community clinic initiatives in the country. Though they are not much in the limelight because of the distance from Delhi, initial reports suggest that basti dawakhanas are equally popular. The outcome of these two initiatives can change the way States and urban local bodies plan primary health services and prompt more States to take such initiatives to strengthen primary healthcare.
Reforms in medical education: The decision for revision in MBBS curriculum, with inclusion of courses on attitude, ethics and communication, was undertaken last year. The revised curriculum, the first after 21 years, will be implemented from the 2019-20 academic year. This comes at a time when issues of unethical practices in medicine and violence against doctors are gaining ground, a phenomenon documented in the book, Healers or Predators?: Healthcare Corruption in India, written by Samiran Nundy, Keshav Desiraju and Sanjay Nagral. The other pending reform concerns the Medical Council of India through the National Medical Commission Bill, which is still awaiting discussion in Parliament. In 2019, there is a need for consensus among political parties to reform healthcare education and delivery systems to root out corruption.
Tackling air pollution to make air breathable: In India, air pollution is a major risk factor for both acute and chronic respiratory diseases. It is documented as a key aggravator in a 2017 study on the state-level burden of diseases in the country. However, for the third year in a row, air quality has grabbed national and global headlines. The air quality index continues to be a cause of serious concern.
Air pollution is not limited to Delhi or north India but cities across the country have poor air quality with around 70 cities breathing bad as India undergoes a huge infrastructure overhaul. It has been estimated that if air quality standards meet global standards, people in India would live 1.7 to 3.0 years longer. The National Clean Air Programme (NCAP) was launched in India in April 2018, with a plan to reduce air pollution in 100 identified cities. It is now proven that efforts on improving air quality will be a high return investment in the form of better health, higher worker productivity and increased life expectancy. So this year, there is a need for developing multi-sectoral interventions, led by Prime Minister Narendra Modi and Chief Ministers of various States, for clean air. After October 2019, the phase II of ‘Swachh Bharat Mission’ can very well be focussed on ‘Clean air for all.’
Opportunities ahead: The year ahead is an opportunity for India to show global leadership in health. In September, the United Nations General Assembly (UNGA) will hold its 74th session on universal health coverage (UHC). Also, the World Health Organisation’s (WHO) annual World Health Day 2019 theme is around UHC with a focus on primary healthcare. These are additional opportunities for the country to assume a leadership role in advancing UHC, accelerate implementation of ongoing initiatives and work upon strengthening the healthcare system, by providing attention on all aspects.
The momentum generated in the last two years, the high political and public visibility of Ayushman Bharat and the competition among States to better their healthcare records are positive peaks in the graph. For long, healthcare and education have been on the lower spectrum of allocations of the GDP. Hope we look at these crucial asset sectors and push up our development indices.
(The writer is a leading public health expert based in New Delhi)
Writer: Chandrakant Lahariya
Courtesy: The Pioneer

Indian Rural Healthcare in Sorry State
by Daljit Singh/Anjan Bose / 09 July 2018Rural areas in India is reeling under acute shortage of physicians and lack of proper healthcare infrastructure. Only when we learn from our failures can we do a course correction.
As a part of the Sustainable Development Goals (SDG), India committed to achieve Universal Health Coverage (UHC). However, its total healthcare expenditure (under five percent of its GDP) resulted in sub-optimal outcomes. With less spending, India faces a severe shortage of hard infrastructure and talent along with regional imbalances in healthcare delivery. Although rural India accounts for about 70 percent of the population, it has less than one-third of nation’s hospitals, doctors and beds, resulting in large disparities in health outcomes across States.
As India’s health system faces multipronged challenges, deficiency of doctors has emerged as one of the biggest roadblocks in the making of a new healthcare ecosystem. Currently, there is a shortfall of nearly two million doctors and four million nurses. Moreover, doctors’ numbers are also skewed towards a few States. According to NATHEALTH’s Aarogya Bharat Report- “India Healthcare Roadmap for 2025”, healthcare services are expected to generate demand for 15 million to 20 million new jobs for doctors and other health professionals by 2025. In spite of such huge prospects, India continues to face severe shortage.
India has less than one doctor for every 1,000 citizens, which is less than the World Health Organisation (WHO) standard that prescribes a doctor population ratio of 1:1,000. If Ayush practitioners are included, India has 1.3 doctors for 1000 population. A Medical Council of India (MCI) report suggests that in July 2017, there were a total 10,22,859 allopathic doctors registered with the MCI or with state medical councils. As per the Aarogya Bharat Report, the shortfall of doctors is likely to continue till 2039. India is passing through a critical phase, and to deal with the situation, it needs urgent structural reforms.
National Medical Commission — managing it professionally: India needs to be in mission mode to bridge the critical gap in available health professionals. The Government is all set to restructure the way India manages the supply side of medical professionals. The National Medical Commission (NMC) Bill, which is expected to be tabled in the Parliament during the monsoon session, will address several issues related to doctors’ deficiency. It is promising to note that the Government has carefully dealt with the concerns expressed by the Indian Medical Association (IMA) and other experts and their suggestions were incorporated to modify the Bill, which was approved by the Cabinet early this year.
Issues related to screening tests for doctors with foreign medical qualifications, “bridge course” for Ayush practitioners to practise modern medicine, fees and seats by private institutions have also been resolved. Apart from scope, the constitution of the Commission has also been restructured with number of nominees from States and Union Territories in the NMC going up to six from three. To give it a professional character, the NMC will comprise 25 members, of which, at least 21 will be doctors.
Pride of medical professionals: The pride and status of medical professionals of all cadres is waning. There is an utter disregard for the attempts to provide basic amenities to doctors in rural areas. Apathetic management for staff and lack of professional protection during healthcare delivery further aggravates the problem. This holds back healthcare providers to take innovative steps suitable for local needs. There is an absence of reward for excellence or punishment for failures in the system.
In order to cope up with ‘doctors’ deficiency’ in rural areas, the Governments must develop model villages and blocks. The concept of model group housing at block level or primary healthcare level should be considered, where Government employees of all departments could be provided accommodation and required facilities like school, playground, community centre, supermarket et al could be bestowed in the neighbourhood. This concept would allow holding, retaining and recruiting fresh talent by facilitating their stay and improvising their quality of life comparable with their counterparts in the city.
The way forward: Prioritising areas with critical shortage of healthcare professionals especially doctors will be important. Moreover, regulations that enable private participation in medical education need to be created. Exploring public-private partnership (PPP) models to enable a rapid increase in medical education seats needs to be given priority. Focusing on primary care can help reduce hospitalisation rates. And telemedicine and remote monitoring tools can be used to widen the reach of existing doctors and increase their productivity. The implementation of Pradhan Mantri Rashtriya Swasthya Suraksha Scheme under Ayushman Bharat Mission, clearly indicates that Prime Minister Narendra Modi, with innovative doable solutions, prefers to act as a radical plastic surgeon rather than the cosmetic one, to change the lives of rural ailing population. ‘Doctors’ deficiency’ remains a big challenge and to fulfil the dream of ‘Swasth Bharat’ (Healthy India), this has to be taken up by all stakeholders on an urgent basis.
Writer: Daljit Singh/Anjan Bose
Courtesy: The Pioneer

PMRSSM: A New Initiative by Government in Healthcare
by Ashwini Kumar Chawbey / 25 May 2018The Pradhan Mantri Rashtriya Swasthya Suraksha Mission is a new and groundbreaking initiative of the Government which aims at providing easily available medical insurance and health services to the poor
It is extremely worrying that nearly 60 million Indians are pushed into poverty because they are, unfortunately, compelled to shell out half of their annual household expenditure to meet medical needs, especially when it comes to hospitalisation. Even after 70 years of independence, there is no real health insurance scheme for 80 per cent of the Indian population.
One of the major healthcare scheme, ‘Ayushman Bharat’, announced by the Union Government in this year’s Budget, is as a game-changer. It aims to ensure better healthcare to the people, particularly from the lower strata of the society. The scheme has two components — the Pradhan Mantri Rashtriya Swasthya Suraksha Mission (PMRSSM) and health and wellness centres. The PMRSSM, a mega healthcare scheme, aims to provide free health treatment up to five lakh rupees to the poor and vulnerable sections of the society. More than 10 crore identified families, covering more than 50 crore, are entitled to benefit under this mission.
For a focused approach and better implementation of the scheme, a dedicated society, called the National Health Agency (NHA), has been formed to administer and implement the PMRSSM under the Ministry of Health & Family Welfare.
As a first step, to roll out the PMRSSM, several Memorandum of Understandings (MoUs) have been signed between four States — Himachal Pradesh, Haryana, Jammu & Kashmir, Uttarakhand and Union Territory of Chandigarh with the National Health Agency. Rest of the States are expected to follow suit soon.
PMRSSM is expected to provide cashless and paperless access to services for the beneficiary at both public and private empanelled hospitals across the country. There will be no capping on family size. This will ensure that all members of designated families, specifically girl child and senior citizens, get maximum coverage.
Besides, preference is also being accorded to make woman as the head of the family to ensure gender justice. More than 1,300 medical packages have been defined, that covers surgery, medical and day care treatments, including medicines, diagnostics, among others.
The PMRSSM is designed on entitlement basis. This means every family figuring in defined Socio Economic Caste Census (SECC), 2011 database will be entitled to claim benefit under the scheme. States will have an option to use an existing trust/society/not-for-profit organistaion or set up a new trust/society/NGO.
States will also be at liberty to choose the modalities for implementation. They can implement scheme through insurance company or directly through the trust/society or a mixed model.
Notably, a well-defined complaint and public grievance redressal mechanism will be instituted, actively utilising electronic, mobile platform, Internet as well as social media and robust safeguards to prevent misuse, fraud or abuse by providers and users. Pre-authorisation will be made mandatory for all tertiary care and selected secondary care packages.
Almost 1.50 lakh primary healthcare centres across the country will be upgraded and well-equipped with diagnostics, drugs and doctors laying the foundation of India’s new healthcare system. These centres aim for early detection of diseases. Universal health checkup will be ensured of every individual before they attain 30 years of age.
The Government enlists cooperation of State Governments in the true spirit of cooperative federalism, insurance companies, hospitals and diagnostic centres, pharma companies, health fund managers and the corporates. This will transform Indian health sector in a significant manner as it will make healthcare easily accessible and effective to the poorest of the poor. It is the need of the hour.
(The writer is Union Minister of State for Health and Family Welfare)
Writer: Ashwini Kumar Chawbey
Courtesy: The Pioneer

Traditional Stress Busters
by Dr. Sanjeev Kumar Pandey / 01 October 2012Our planet - The Earth has conducive atmosphere for life in our solar system by virtue of ecological balance between Living & Nonliving and Flora & Fauna, since the evolution began.
Living ones have been provided with 4 natural instinct and 'Indris' for use of resources provided by Nature to live healthy life span ,to continue the progeny and peaceful passing away for recycling of energy.
One species of living kingdom brought about tremendous changes and developed one more tool - Intellect. By using intellect, they developed at much faster pace than other living being - they are referred to as Homo Sapiens- Most Advance Auto-programmed computer of our planet - HUMAN BEING'.
Human being established harmony with Nature- by framing Basics rules of Lifestyle to restore stress free life on wheels of spirituality.
By virtue of wisdom, since ancient time, visionary people visualized STRESS ( Physical , Mental & Oxidative) is an instrumental component , which governs the human health.
STRESS
- To a lay man :Stress is a situation which causes emotional upset & tension
- To a Psychiatrist : Stress is a situation which alters the psychological haemostatic process.
- To a Anthropologist : Stress is an adversity between people & environment.
- According to Hans Selye (Endocrinologist) : Stress is a non specific response of the body to any demand made on it.
The food plays an important in managing stress, specially, Oxidative STRESS, the most damaging type of stress - it may cause Cancer, Auto-immune disease by gene mutation, Diabetes, Arthritis, Osteoporosis Libido, Hypertension even Psychiatric disorders, if goes beyond the thresh-hold limit .
(1) Yogic Food: The Yogic food are those edible substances, which are available for meal as good as in natural form accordance to particular geographical conditions, environment & season. Brief Scientific deliberation about Oxidative Stress.
The Human being existence is not possible without energy, produced by food digestion in intestine with help of enzymatic reaction and combustion at cellular level in both processes can't be takes place without oxygen. The oxygen content of air has its negative character for living organism. After reacting with other element in body at cellular level produces- the super oxide radical, hydrogen peroxide & extremely reactive hydroxyl radicals are common. The radicals are responsible for oxygen toxicity
(2). These radicals are known as free radicals. More complex food - more enzymatic - more oxygen requirement and in result more free radicals formation creates the Oxidative Stress. The oxidative stress damages the cell membrane, DNA, precipitate as chronic disease or problem, whenever the amount of radical cross beyond control of inbuilt defense mechanism. All living beings generate water & lipidsoluble antioxidants & syn- thesized antioxidant enzymes called as Super Oxides Dismutase(SOD) to nullify the reactive oxygen free radicals
(3). To deal with oxidative damage number of repair enzymes produce in the body for proteins, lipids & DNA repair (4). The oxidative stress is non-static, always fluctuate, God, provided the human being the adaptation mechanism to deal with such fluctuating stressors by initiating antioxidants & damage repair/removal enzymes
(4). Traditional Management to Deal with Oxidative Stress
By virtue of wisdom, since ancient time, visionary people visualized an individual is compel to face stress, unknowingly off course willingly too. The body is capable of maintaining the internal environment with in very narrow range called 'Normal Range'. For example in Hindu Mythology - Frame an unique 9 day systematic religious fasting system biyearly during Navratri ( In April & October ) along with deferent mode of worship.
For fasting period, visionary people have laid down guidelines for the meal pattern & food item restriction and linked them with religious Astha, so, community in mass can fallow that and remain healthy, manpower can contribute at optimum level in development..
In April & October month, the season in under window period of change from winter to summer, summer to winter-The Human body is in process of making adjustment according to change in outer environment, so many chemical reaction are going on , In result heavy amount free radical are being produced and body self mechanism busy to deal with these free radical to keep the oxidative stress with threshhold limit.
So, any kind of extra demand made on body may lead produce more free radical taking oxidative stress beyond threshold limit, may leads to any permanent damage or chronic aliments or acute ailments may convert in chronic one.
Prescribed Meal pattern & food item during, fasting period
Meditation: The meditation is not only few minute state of closed eye static posture but it is a state of meditative posture throughout the day to keep the Central Nervous system in proper order to achieve the positive health i.e. Mental, Physical, Social & spiritual health.
- Worship / Reading Religious Original Text - This is a type of Meditation , lowers BMI , conserves energy - Lower the Free radical production .
- Sat Sang: Bests stress reliever activity - Lower the free radical production.
- Meditation: Help in taking voluntary control over involuntary physiology activities.
- Fruits: Provide simplest form of glucose ( fructose - ready energy)., Vitamins , Minerals ( as anti oxidants , Roughs -good for cleaning GIT & help in clearing bowel. And Potassium for lowering stress at cellular level
- Dry Fruits: Provides essential oil, minerals, Vitamins required in traces, for skin & visceral muscles toning
- Vegetable: Are calories free food item which provides plenty of water, vitamins, minerals lowers the burden of digestion & combustion - minimizes free radical production.
- Spices: Clove (Syzygium Aromaticum) - provides oral hygiene, prevention from clod & cough & Cardamom (Elettaria cardamomu ) - Checks the acidity problem, help in digestion, & works as mouth Freshener.
- Rock Salt: Rock salt provides high Potassium & low Sodium - it releases the internal fluid stress on cell membrane & lower the chances on untamed death of cell from rapture.It help to the functioning of sodium potassium pump at cell membrane.
Problem of today: In today's world, very scientific concept of bi-yearly fasting formula to keep healthy life, taken either as fashion or mistaken or wrongly taken people taking more heavy or taking no food or not aware about biological base of concept.
Conclusion: Fasting is an activity, to provide space to our body systems to rearrange the physiological activities to you away fro so many ailments at same time provides you healthy life & economy, formulated by visionary people .
Suggestion : Due to hectic life schedules, environmental imbalance, irrational use of medicines the level of Oxidative Stress is much higher in human body .
So, weekly fasting is advisable.
(Writer is a Lucknow-based naturopathy consutant)

Traditional Stress Busters
by Opinion Express / 01 October 2012Our planet - The Earth has conducive atmosphere for life in our solar system by virtue of ecological balance between Living & Nonliving and Flora & Fauna, since the evolution began. Living ones have been provided with 4 natural instinct and 'Indris' for use of re- sources provided by Nature to live healthy life span ,to continue the progeny and peaceful passing away for recycling of energy.
One species of living kingdom brought about tremendous changes and developed one more tool - Intellect. By using intellect, they developed at much faster pace than other living being - they are re- ferred to as Homo Sapiens- Most Advance Auto-programmed computer of our planet 'HUMAN BEING'. Human being established harmony with Nature- by framing Basics rules of Lifestyle -to restore stress free life on wheels of spirituality.
By virtue of wisdom, since ancient time, visionary people visualized STRESS ( Physical , Mental & Oxidative) is an instrumental component, which governs the human health.
STRESS
- To a lay man: Stress is a situation which causes emotional upset & tension.
- To a Psychiatrist: Stress is a situation which alters the psychological haemostatic process.
- To a Anthropologist: Stress is an adversity between people & environment.
- According to Hans Selye (Endocrinologist): Stress is a non specific response of the body to any demand made on it.
The food plays an important in managing stress, specially, Oxidative STRESS,the most damaging type of stress - it may cause - Cancer, Auto-immune disease by gene mutation, Diabetes, Arthritis, Osteoporosis Libido, Hypertension even Psychiatric disorders, if goes beyond the thresh-hold limit.
(1) Yogic Food: The Yogic food are those edible substances ,which are available for meal as good as in natural form accordance to particular geographical conditions, environment & season.
Brief Sientific deliberation about Oxidative Stress
The Human being existence is not possible without energy, produced by food digestion in intestine with help of enzymatic reaction and combustion at cellular level in both processes can't be takes place without oxygen. The oxygen content of air has its negative character for living organism .After reacting with other element in body at cellular level produces- the super oxide radical, hydrogen peroxide & extremely reactive hydroxyl radicals are common, The radicals are responsible for oxygen toxicity
(2). These radicals are known as free radicals.
More complex food more enzymatic more oxygen requirement and in result more free radicals formation creates the Oxidative Stress.
The oxidative stress damages the cell membrane, DNA, precipitate as chronic disease or problem, whenever the amount of radical cross beyond control of inbuilt defense mechanism. All living beings generate water & lipid- soluble antioxidants & synthesized antioxidant enzymes called as Super Oxides Dismutase(SOD) to nullify the reactive oxygen free radicals
(3). To deal with oxidative damage number of repair enzymes produce in the body for proteins, lipids & DNA repair
(4). The oxidative stress is non-static, always fluctuate, provided the human being the adaptation mechanism to deal with such fluctuations
Religious activity
- Worship
- Reading Religious Books
- Sat sang
- Meditation
Meal Pattern
2 times /day But last meal before sunset
Food Item
- Fruits (seasonal)
- Dry Fruits
- Vegetable (Seasonal)
- Spices (Clove, Cardamom)
- Rock Salting stressors by initiating antioxidants & damage repair/removal enzymes
(4). Traditional Management to Deal with Oxidative Stress
By virtue of wisdom, since ancient time, visionary people visualized an individual is compel to face stress, unknowingly off course willingly too. The body is capable of maintaining the internal environment with in very narrow range called 'Normal Range'. For example in Hindu Mythology - Frame an unique 9 day systematic religious fasting system bi-yearly during Navratri ( In April & October ) along with deferent mode of worship.
For fasting period, visionary people have laid down guidelines for the meal pattern & food item restriction and linked them with religious Astha, so community in mass can fallow that and remain healthy, manpower can contribute at optimum level in development.
In April & October month, the season in under window period of change from winter to summer, summer to winter, The Human body is in process of making adjustment according to change in outer environment, so many chemical reaction are going on, In result heavy amount free radical are being produced and body self mechanism busy to deal with these free radical to keep the oxidative stress with thresh-hold limit.
So, any kind of extra demand made on body may lead produce more free radical taking oxidative stress beyond threshold limit, may leads to any permanent damage or chronic aliments or acute ailments may convert in chronic one. Prescribed Meal pattern & food item during, fasting period.
Meditation: The meditation is not only few minute state of closed eye static posture but it is a state of meditative posture throughout the day to keep the Central Nervous system in proper order to achieve the positive health i.e. Mental, Physical, Social & spiritual health.
- Worship / Reading Religious Original Text -
This is a type of Meditation , lowers BMI , conserves energy - Lower the Free radical production .
- Sat Sang: Bests stress reliever activity - Lower the free radical production.
- Meditation: Help in taking voluntary control over involun- tary physiology activities.
- Fruits: Provide simplest form of glucose ( fructose - ready energy)., Vitamins , Minerals ( as anti oxidants , Roughs -good for cleaning GIT & help in clearing bowel. And Potassium for lower- ing stress at cellular level
- Dry Fruits: Provides essential oil , minerals , Vitamins re- quired in traces , for skin & visceral muscles toning
- Vegetable: Are calories free food item which provides plenty of water , vitamins , minerals
Lowers the burden of digestion & combustion - minimizes free radical production.
- Spices : Clove (Syzygium Aromaticum) provides oral hygiene, prevention from clod & cough & Cardamom (Elettaria cardamomu ) - Checks the acidity problem, help in digestion & works as mouth Freshener
- Rock Salt: Rock salt provides high Potassium & low Sodium - it releases the internal fluid stress on cell membrane & lower the chances on untamed death of cell from rapture.It help to the functioning of sodium potassium pump at cell membrane.
Problem of today: In today's world, very scientific concept of bi-yearly fasting formula to keep healthy life, taken either as fashion or mistaken or wrongly taken people taking more heavy or taking no food or not aware about biological base of concept.
Conclusion: Fasting is an activity, to provide space to our body systems to rearrange the physiological activities to you away from so many ailments at same time provides you healthy life & economy, formulated by visionary people. Suggestion: Due to hectic life schedules , environmental im- balance, irrational use of medicines the level of Oxidative Stress is much higher in human body. So, weekly fasting is advisable.
(Writer is a Lucknow-based naturopathy consutant)

Diet & Nutrition is key to Healthy Living
by Vivek Dubey / 01 April 2012Indian tends to ignore the importance of diet & nutrition in their daily life. The problem is acute at the primary stage of life wherein Indian parents are obsessed with education priority ignoring health aspect. Indian women are largely ignorant on dietary issues making themselves victim of lifestyle diseases.
Healthy eating is not about strict nutrition philosophies, staying unrealistically thin, or depriving yourself of the foods you love. Rather, it’s about feeling great, having more energy, and keeping yourself as healthy as possible– all of which can be achieved by learning some nutrition basics and using them in a way that works for you.
Healthy eating begins with learning how to “eat smart”—it’s not just what you eat, but how you eat. Your food choices can reduce your risk of illnesses such as heart disease, cancer, and diabetes, as well as defend against depression. Additionally, learning the habits of healthy eating can boost your energy, sharpen your memory and stabilize your mood. You can expand your range of healthy food choices and learn how to plan ahead to create and maintain a satisfying, healthy diet.
Healthy eating tip 1: Set yourself up for success
To set yourself up for success, think about planning a healthy diet as a number of small, manageable steps rather than one big drastic change. If you approach the changes gradually and with commitment, you will have a healthy diet sooner than you think.
Simplify. Instead of being overly concerned with counting calories or measuring portion sizes, think of your diet in terms of color, variety, and freshness. This way it should be easier to make healthy choices. Focus on finding foods you love and easy recipes that incorporate a few fresh ingredients. Gradually, your diet will become healthier and more delicious. Start slow and make changes to your eating habits over time.
Trying to make your diet healthy overnight isn’t realistic or smart. Changing everything at once usually leads to cheating or giving up on your new eating plan. Make small steps, like adding a salad (full of different color vegetables) to your diet once a day or switching from butter to olive oil when cooking. As your small changes become habit, you can continue to add more healthy choices to your diet.
Every change you make to improve your diet matters. You don’t have to be perfect and you don’t have to completely eliminate foods you enjoy to have a healthy diet. The long term goal is to feel good, have more energy, and reduce the risk of cancer and disease. Don’t let your missteps derail you— every healthy food choice you make counts. Think of water and exercise as food groups in your diet.
Water: Water helps flush our systems of waste products and toxins, yet many people go through life dehydrated—causing tiredness, low energy, and headaches. It’s common to mistake thirst for hunger, so staying well hydrated will also help you make healthier food choices.
Exercise: Find something active that you like to do and add it to your day, just like you would add healthy greens, blueberries, or salmon. The benefits of lifelong exercise are abundant and regular exercise may even motivate you to make healthy food choices a habit.
Healthy eating tip 2: Moderation is key
People often think of healthy eating as an all or nothing proposition, but a key foundation for any healthy diet is moderation. Despite what certain fad diets would have you believe, we all need a balance of carbohydrates, protein, fat, fiber, vitamins, and minerals to sustain a healthy body.
Try not to think of certain foods as “off-limits.” When you ban certain foods or food groups, it is natural to want those foods more, and then feel like a failure if you give in to temptation. If you are drawn towards sweet, salty, or unhealthy foods, start by reducing portion sizes and not eating them as often. Later you may find yourself craving them less or thinking of them as only occasional indulgences. Think smaller portions. Serving sizes have ballooned recently, particularly in restaurants. When dining out, choose a starter instead of an entrée, split a dish with a friend, and don’t order supersized anything. At home, use smaller plates, think about serving sizes in realistic terms, and start small. Visual cues can help with portion sizes—your serving of meat, fish, or chicken should be the size of a deck of cards. A teaspoon of oil or salad dressing is about the size of a matchbook and your slice of bread should be the size of a CD case.
Healthy eating tip 3: It's not just what you eat, it's how you eat
Healthy eating is about more than the food on your plate—it is also about how you think about food. Healthy eating habits can be learned and it is important to slow down and think about food as nourishment rather than just something to gulp down in between meetings or on the way to pick up the kids.
Eat with others whenever possible. Eating with other people has numerous social and emotional benefits—particularly for children—and allows you to model healthy eating habits. Eating in front of the TV or computer often leads to mindless overeating. Take time to chew your food and enjoy mealtimes. Chew your food slowly, savoring every bite. We tend to rush though our meals, forgetting to actually taste the flavors and feel the textures of our food. Reconnect with the joy of eating. Listen to your body. Ask yourself if you are really hungry, or have a glass of water to see if you are thirsty instead of hungry. During a meal, stop eating before you feel full. It actually takes a few minutes for your brain to tell your body that it has had enough food, so eat slowly. Eat breakfast, and eat smaller meals throughout the day. A healthy breakfast can jumpstart your metabolism, and eating small, healthy meals throughout the day (rather than the standard three large meals) keeps your energy up and your metabolism going.
Healthy eating tip 4: Fill up on colorful fruits and vegetables
Fruits and vegetables are the foundation of a healthy diet. They are low in calories and nutrient-dense, which means they are packed with vitamins, minerals, antioxidants, and fiber.
Try to eat a rainbow of fruits and vegetables every day and with every meal—the brighter the better. Colorful, deeply colored fruits and vegetables contain higher concentrations of vitamins, minerals, and antioxidants—and different colors provide different benefits, so eat a variety. Aim for a minimum of five portions each day.
Some great choices include:
Greens: Branch out beyond bright and dark green lettuce. Kale, mustard greens, broccoli, and Chinese cabbage are just a few of the options—all packed with calcium, magnesium, iron, potassium, zinc, and vitamins A, C, E, and K.
Sweet vegetables: Naturally sweet vegetables—such as corn, carrots, beets, sweet potatoes, yams, onions, and squash—add healthy sweetness to your meals and reduce your cravings for other sweets.
Fruit: Fruit is a tasty, satisfying way to fill up on fiber, vitamins, and antioxidants. Berries are cancer-fighting, apples provide fiber, oranges and mangos offer vitamin C, and so on.
The importance of getting vitamins from food—not pills
The antioxidants and other nutrients in fruits and vegetables help protect against certain types of cancer and other diseases. And while advertisements abound for supplements promising to deliver the nutritional benefits of fruits and vegetables in pill or powder form, research suggests that it’s just not the same.
A daily regimen of nutritional supplements is not going to have the same impact of eating right. That’s because the benefits of fruits and vegetables don’t come from a single vitamin or an isolated antioxidant.
The health benefits of fruits and vegetables come from numerous vitamins, minerals, and phytochemicals working together synergistically. They can’t be broken down into the sum of their parts or replicated in pill form.
Healthy eating tip 5: Eat more healthy carbs and whole grains
Choose healthy carbohydrates and fiber sources, especially whole grains, for long-lasting energy. In addition to being delicious and satisfying, whole grains are rich in phytochemicals and antioxidants, which help to protect against coronary heart disease, certain cancers, and diabetes. Studies have shown people who eat more whole grains tend to have a healthier heart.
A quick definition of healthy carbs and unhealthy carbs
Healthy carbs (sometimes known as good carbs) include whole grains, beans, fruits, and vegetables. Healthy carbs are digested slowly, helping you feel full longer and keeping blood sugar and insulin levels stable.
Unhealthy carbs (or bad carbs) are foods such as white flour, refined sugar, and white rice that have been stripped of all bran, fiber, and nutrients. Unhealthy carbs digest quickly and cause spikes in blood sugar levels and energy.
Tips for eating more healthy carbs
Include a variety of whole grains in your healthy diet, including whole wheat, brown rice, millet, quinoa, and barley. Experiment with different grains to find your favorites.
Make sure you're really getting whole grains. Be aware that the words stone-ground, multi-grain, 100% wheat, or bran can be deceptive. Look for the words “whole grain” or “100% whole wheat” at the beginning of the ingredient list. In the U.S., check for the Whole Grain Stamps that distinguish between partial whole grain and 100% whole grain.
Try mixing grains as a first step to switching to whole grains. If whole grains like brown rice and whole-wheat pasta don’t sound good at first, start by mixing what you normally use with the whole grains. You can gradually increase the whole grain to 100%.
Avoid: Refined foods such as breads, pastas, and breakfast cereals that are not whole grain.
Healthy eating tip 6: Enjoy healthy fats & avoid unhealthy fats
Good sources of healthy fat are needed to nourish your brain, heart, and cells, as well as your hair, skin, and nails. Foods rich in certain omega-3 fats called EPA and DHA are particularly important and can reduce cardiovascular disease, improve your mood, and help prevent dementia.
Add to your healthy diet:
Monounsaturated fats, from plant oils like canola oil, peanut oil, and olive oil, as well as avocados, nuts (like almonds, hazelnuts, and pecans), and seeds (such as pumpkin, sesame).
Polyunsaturated fats, including Omega-3 and Omega -6 fatty acids, found in fatty fish such as salmon, herring, mackerel, anchovies, sardines, and some cold-water fish oil supplements. Other sources of polyunsaturated fats are unheated sunflower, corn, soybean, flaxseed oils, and walnuts.
Reduce or eliminate from your diet:
Saturated fats, found primarily in animal sources including red meat and whole-milk dairy products.
Trans fats, found in vegetable shortenings, some margarines, crackers, candies, cookies, snack foods, fried foods, baked goods, and other processed foods made with partially hydrogenated vegetable oils.
Healthy eating tip 7: Put protein in perspective
Protein gives us the energy to get up and go and keep going. Protein in food is broken down into the 20 amino acids that are the body’s basic building blocks for growth and energy, and essential for maintaining cells, tissues, and organs. A lack of protein in our diet can slow growth, reduce muscle mass, lower immunity, and weaken the heart and respiratory system. Protein is particularly important for children, whose bodies are growing and changing daily.
Here are some guidelines for including protein in your healthy diet:
Try different types of protein. Whether or not you are a vegetarian, trying different protein sources—such as beans, nuts, seeds, peas, tofu, and soy products—will open up new options for healthy mealtimes.
Beans: Black beans, navy beans, garbanzos, and lentils are good options.
Nuts: Almonds, walnuts, pistachios, and pecans are great choices.
Soy products: Try tofu, soy milk, tempeh, and veggie burgers for a change.
Avoid salted or sugary nuts and refried beans.
Downsize your portions of protein. Many people in the West eat too much protein. Try to move away from protein being the center of your meal. Focus on equal servings of protein, whole grains, and vegetables.
Focus on quality sources of protein, like fresh fish, chicken or turkey, tofu, eggs, beans, or nuts. When you are having meat, chicken, or turkey, buy meat that is free of hormones and antibiotics.
Healthy eating tip 8: Add calcium for strong bones
Calcium is one of the key nutrients that your body needs in order to stay strong and healthy. It is an essential building block for lifelong bone health in both men and women, as well as many other important functions.
You and your bones will benefit from eating plenty of calcium-rich foods, limiting foods that deplete your body’s calcium stores, and getting your daily dose of magnesium and vitamins D and K— nutrients that help calcium do its job.
Recommended calcium levels are 1000 mg per day, 1200 mg if you are over 50 years old. Take a vitamin D and calcium supplement if you don’t get enough of these nutrients from your diet.
Good sources of calcium include:
Dairy: Dairy products are rich in calcium in a form that is easily digested and absorbed by the body. Sources include milk, yogurt and cheese.
Vegetables and greens: Many vegetables, especially leafy green ones, are rich sources of calcium. Try turnip greens, mustard greens, collard greens, kale, romaine lettuce, celery, broccoli, fennel, cabbage, summer squash, green beans, Brussels sprouts, asparagus, and crimini mushrooms.
Beans: For another rich source of calcium, try black beans, pinto beans, kidney beans, white beans, black-eyed peas, or baked beans.
Healthy eating tip 9: Limit sugar and salt
If you succeed in planning your diet around fiber-rich fruits, vegetables, whole grains, lean protein, and good fats, you may find yourself naturally cutting back on foods that can get in the way of your healthy diet—sugar and salt.
Sugar
Sugar causes energy ups and downs and can add to health and weight problems. Unfortunately, reducing the amount of candy, cakes, and desserts we eat is only part of the solution. Often you may not even be aware of the amount of sugar you’re consuming each day. Large amounts of added sugar can be hidden in foods such as bread, canned soups and vegetables, pasta sauce, margarine, instant mashed potatoes, frozen dinners, fast food, soy sauce, and ketchup. Here are some tips:
Avoid sugary drinks: One 12-oz soda has about 10 teaspoons of sugar in it, more than the daily recommended limit! Try sparkling water with lemon or a splash of fruit juice.
Eat naturally sweet food such as fruit, peppers, or natural peanut butter to satisfy your sweet tooth.
How sugar is hidden on food labels Check food labels carefully. Sugar is often disguised using terms such as:
Cane sugar or maple syrup: crystallized or evaporated cane juice
Corn sweetener or corn syrup: fruit juice concentrates, such as apple or pear
Honey or molasses: maltodextrin (or dextrin)
Brown rice syrup: Dextrose, Fructose, Glucose, Maltose, or Sucrose
Salt
Most of us consume too much salt in our diets. Eating too much salt can cause high blood pressure and lead to other health problems. Try to limit sodium intake to 1,500 to 2,300 mg per day, the equivalent of one teaspoon of salt.
Avoid processed or pre-packaged foods. Processed foods like canned soups or frozen dinners contain hidden sodium that quickly surpasses the recommended limit.
Be careful when eating out. Most restaurant and fast food meals are loaded with sodium.
Opt for fresh or frozen vegetables instead of canned vegetables.
Cut back on salty snacks such as potato chips, nuts, and pretzels.
Choose low-salt or reduced-sodium products.
Try slowly reducing the salt in your diet to give your taste buds time to adjust.
Experts agree the key to healthy eating is the time-tested advice of balance, variety and moderation. In short, that means eating a wide variety of foods without getting too many calories or too much of any one nutrient.
Maintain a healthy weight. The weight that's right for you depends on many factors including your sex, height, age and heredity. Excess body fat increases your chances for high blood pressure, heart disease, stroke, diabetes, some types of cancer and other illnesses. But being too thin can increase your risk for osteoporosis, menstrual irregularities and other health problems. If you're constantly losing and regaining weight, a registered dietitian can help you develop sensible eating habits for successful weight management. Regular exercise is also important to maintaining a healthy weight.
Make changes gradually. Just as there are no "superfoods" or easy answers to a healthy diet, don't expect to totally revamp your eating habits overnight. Changing too much, too fast can get in the way of success. Begin to remedy excesses or deficiencies with modest changes that can add up to positive, lifelong eating habits. For instance, if you don't like the taste of skim milk, try low-fat. Eventually, you may find you like skim, too.
FREE Download
OPINION EXPRESS MAGAZINE
Offer of the Month






